Data Conversion Services
Is an Automated EHR Data Conversion Right for You?
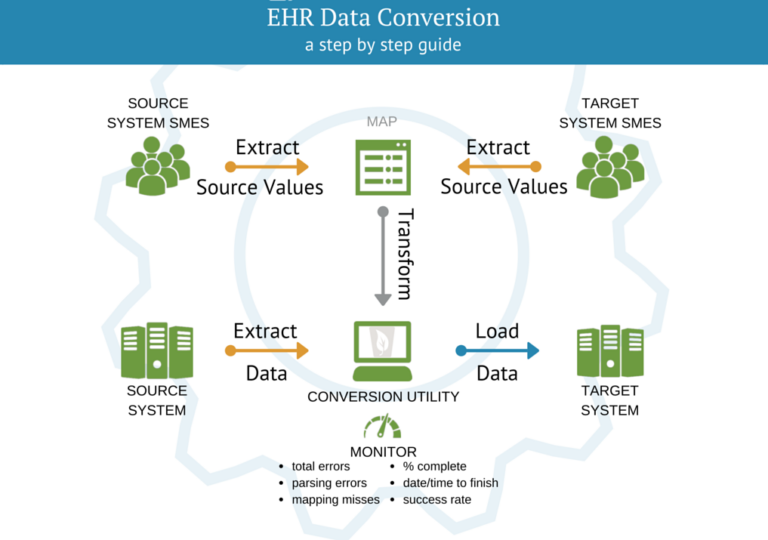
EHR data conversion is the process of taking data from a legacy electronic health record system and transferring it to a new system.EHR data

EHR data conversion is the process of taking data from a legacy electronic health record system and transferring it to a new system.EHR data

Over the last ten years, provider adoption of Electronic Health Records (EHRs) has grown significantly. Healthcare providers are expected to document encounters with patients
By providing my email address to Keystone Technologies, I agree to be contacted for marketing purposes. Please refer to our Privacy Policy for more questions or details.